Infection Control & Prevention in Dentistry
By Kay Carl, RN, BS, Infection Preventionist
After reading this article, the reader should be able to:
- Identify the key reference for infection prevention strategies for dental practice.
- Monitor sterilization practices in the dental setting
- List appropriate immunizations for dental health care workers.
Dental Treatment Innovations
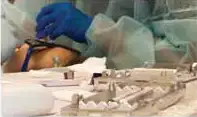 Having been an infection control nurse since the 1970s, now an infection preventionist in the dental field, I find myself being a historian many times. For those of you who read my articles on a regular basis, you know I like to include a summary of what infection control problems we dealt with in the past, what little we had to combat those problems, and what is readily available today. Many times when new technology was introduced, unforeseen problems ensued. For example, air-driven handpieces developed in the 1950s and 1960s increased bur rotation which made treatment faster and less traumatic for the patient. But the increased rotation of the burs generated heat and there was concern that the high temperature could devitalize teeth. Dental researchers tackled this problem and added a water source to the handpiece to serve as a coolant. Then a second problem ensued; the water would drip on the patients during procedures even after the handpiece was turned off. To solve this dilemma, retraction valves were developed and installed in dental units. A third problem arose when large quantities of biofilms formed when the retraction valves sucked contaminated water back into the unit. Finally, check valves or anti-retraction valves were developed to combat this problem. However, we still had dental unit water contamination and at first labor-intensive procedures were needed to combat the biofilms. Now all you have to do is add a tablet to your water bottle each time you fill it or attach a device that should last a whole year.
Having been an infection control nurse since the 1970s, now an infection preventionist in the dental field, I find myself being a historian many times. For those of you who read my articles on a regular basis, you know I like to include a summary of what infection control problems we dealt with in the past, what little we had to combat those problems, and what is readily available today. Many times when new technology was introduced, unforeseen problems ensued. For example, air-driven handpieces developed in the 1950s and 1960s increased bur rotation which made treatment faster and less traumatic for the patient. But the increased rotation of the burs generated heat and there was concern that the high temperature could devitalize teeth. Dental researchers tackled this problem and added a water source to the handpiece to serve as a coolant. Then a second problem ensued; the water would drip on the patients during procedures even after the handpiece was turned off. To solve this dilemma, retraction valves were developed and installed in dental units. A third problem arose when large quantities of biofilms formed when the retraction valves sucked contaminated water back into the unit. Finally, check valves or anti-retraction valves were developed to combat this problem. However, we still had dental unit water contamination and at first labor-intensive procedures were needed to combat the biofilms. Now all you have to do is add a tablet to your water bottle each time you fill it or attach a device that should last a whole year.Medical Advancements
Before we start feeling too frustrated dealing with infection prevention in the dental field, we should look to our healthcare colleagues in medicine. A huge problem in hospitals in the United States has been healthcare associated infections (HAIs). One of the most deadly types of HAIs has been the resulting bloodstream infections since central line catheters were first introduced over a decade ago. These catheters are inserted into large veins to deliver fast acting and lifesaving treatment to patients. Called CLABSIs, Central Line Associated Blood Stream Infections can have a mortality rate of 12% to 25%. Fortunately, In 2009, an estimated 25,000 fewer CLABSIs occurred among patients in ICUs in the United States than in 2001 (a 58% reduction).1 Among the reasons for this decline is the attention to adhering to strict protocols of maximum sterile barrier precautions during insertion and removing the catheters as soon as no longer indicated.2 The goal for many Infection Preventionists is to have zero CLABSIs. On April 1, the CDC (Center for Disease Control and Prevention) published detailed guidelines to address this problem.3 Our dental infection prevention problems pale in comparison. So we have had a lot of two steps forward and one step back advances in dentistry and in healthcare in general. When new technology is introduced, sometimes it has major repercussions that no one predicted, and it takes years to find appropriate solutions. We have been fortunate that there is a very active group among dental manufacturers that works to make infection prevention easier with the development of equipment that can be disinfected, and if needed, sterilized, and materials that can be unit dosed out to patients.
So we have had a lot of two steps forward and one step back advances in dentistry and in healthcare in general. When new technology is introduced, sometimes it has major repercussions that no one predicted, and it takes years to find appropriate solutions. We have been fortunate that there is a very active group among dental manufacturers that works to make infection prevention easier with the development of equipment that can be disinfected, and if needed, sterilized, and materials that can be unit dosed out to patients.OSHA
What happened twenty years ago? The Occupational Safety and Health Administration (OSHA), established in 1970, had been lobbied by healthcare workers since the 1980s to be included under OSHA law for protection from bloodborne diseases. On Dec 6, 1991, the Bloodborne Pathogen Standard was published and became law on June 6, 1992.4 In most government dental facilities, there was little change as staff had already been following the dental guidelines from the CDC and recommendations from the United States Public Health Service (USPHS). But this was new ground for most private dental practices. Previously immune from government regulation, with the exception of malpractice claims from patients and censure from state dental boards for practicing dentistry below the standard of care, the dental community was hit hard by the new law.My most frequently asked question in those first years after the OSHA standard became law was, “What is the law and what do I have to do? ”
THE PRESENT
Presently we must adhere to OSHA law which was updated in 2001 to include sharps injuries prevention. We also should be following recommendations from the USPHS, and CDC dental guidelines that were updated in 1993 and then again in 2003. There was a lot of misinformation with the interpretation of these changes and there still is some today as we try to deal with these changes. However, we have had a lot of time to get it right.Are you up to date on what is required in infection control and prevention in dental practice? You can get the vast majority of what is necessary by reading the current CDC Guidelines for Infection Control in Dental Health-Care Settings --- 2003.5 In contrast to the 1986 CDC dental guidelines that consisted of 6 pages6 and the 12-page 1993 guideline7, this comprehensive 87-page document has included occupational exposure recommendations as required by OSHA and includes updated information from the USPHS. It also contains information from a multitude of infection control related guidelines and recommendations from the CDC and other professional entities such as the Society of Healthcare Epidemiology of America (SHEA) and the Association for Professionals in Infection Control and Epidemiology (APIC). Although the guideline is now close to 7 ½ years old, it remains quite current in all aspects. Reading and following this document will answer many of your questions and assist you in following the necessary steps to maintain a high level of professional practice in infection prevention. I consider it mandatory reading for all dentists and hygienists.
Best Practices
The difference between 2003 and the present is that innovations have been developed to make it easier to follow the standards and guidelines required. We have had all these years to develop best practices so we should be pretty good at it by now. And to my delight, I have been hearing less of, “What do I have to do?” and more of, “I want the best infection (prevention) control for my practice; what can do I to achieve that?” Of course, this also has a major impact on your risk management issues as you reduce risk to your patients and staff. We also are aware that it is much easier to trace infection sources with epidemiology practices today. So use your moral courage to care for your patients at the highest level and you will find it rewarding.CDC Dental Guidelines
Let me address what I feel are some of the high points of the current CDC dental guidelines and what additional information we now have since its publication.Employee Health
There are many facets of an employee health program. The following are major points to implement in your practice if you have not already done so.- Vaccination and testing:
- Hepatitis B Vaccination. Dental health care workers (DHCWs) who may be exposed to bloodborne pathogens during their work must be offered the hepatitis B vaccination series without charge.>
- Hepatitis B Antibody Testing. After the hepatitis B vaccination series has been completed, follow up with antibody testing must be done to see if immunity to the hepatitis B virus (HBV) has been achieved. Ten percent of people vaccinated do not respond from the first vaccination series and only half of that ten percent respond after the second round, so it is important to determine immunity. Once immunity is achieved, the protection is for life. No further testing or boosting is necessary.
- Additional Immunizations.The CDC also recommends that healthcare personnel should have the following immunizations:
- influenza (to be given each flu season). Now many hospitals are requiring mandatory flu shots as a work requirement.
- measles/mumps/rubella. This series is part of recommended childhood immunizations so your employees most likely have already had these shots.
- tetanus/diphtheria/pertussis. Pertussis (whooping cough) remains poorly controlled in the United States so there has been a movement from the CDC to improve immunization coverage in adolescents and adults. There is now a Combined Tetanus, Diphtheria, and Pertussis Vaccine called Tdap that has been on the market since 2005. The Advisory Committee on Immunization Practices (ACIP) recommends a one-time dose of Tdap as soon as feasible to all Healthcare Personnel who have not received Tdap previously.8
- Varicella (chickenpox). Sometimes the younger staff has not been vaccinated for chickenpox nor have they had the disease. If exposed to chickenpox, they have to be restricted from work whether or not they develop the disease. Pregnant women risk harm to their fetus if infected.
- Work restrictions for healthcare personnel (HCP) infected with or occupationally exposed to infectious diseases. In Table 1 of the guidelines, there is a two-page chart that lists major infectious diseases, what work restrictions are required, and the duration of the restriction. This is an excellent tool for you to determine when an employee should or should not work.
- Management of occupational exposures to bloodborne pathogens, including postexposure prophylaxis (PEP). There have been more current USPHS recommendations for PEP since the dental guidelines were released, but these are directed to the Occupational Health Providers who treat the exposed employee. So as long as your staff is directed to an appropriate provider for treatment, you do not need to be up on the medical treatment for postexposure.
 Hand-hygiene products and surgical hand antisepsis. The dental guidelines address advances in hand hygiene that are detailed in the CDC hand hygiene guidelines of 2002.9 The guidelines address these issues and also include comments on lotions, fingernails, and jewelry. Dentistry is slowly converting to waterless systems that use alcohol hand rubs. These rubs reduce damage to hands, have a more rapid and effective antimicrobial action than soap and water, and include a residual action. As dentists routinely wash their hands more frequently than general surgeons, the rubs hold a distinctive advantage over soap and water.
Hand-hygiene products and surgical hand antisepsis. The dental guidelines address advances in hand hygiene that are detailed in the CDC hand hygiene guidelines of 2002.9 The guidelines address these issues and also include comments on lotions, fingernails, and jewelry. Dentistry is slowly converting to waterless systems that use alcohol hand rubs. These rubs reduce damage to hands, have a more rapid and effective antimicrobial action than soap and water, and include a residual action. As dentists routinely wash their hands more frequently than general surgeons, the rubs hold a distinctive advantage over soap and water.Contact dermatitis and latex hypersensitivity.
These issues are covered extensively in the guideline.
We first struggled with the use of gloves and then had to deal with the poor quality of what was available in the 90s. These concerns have been met and solved with advances in glove manufacturing that provide a variety of gloves in addition to latex and have fewer irritating substances left in the glove from processing methods.
Dental water-quality concerns. As first mentioned in this article, we now have easier solutions for controlling dental water quality. What we have not achieved is routine testing to confirm the results of our dental water treatment. This we have to work on. In addition to addressing dental water treatment, the guidelines include information to deal with community boil-water advisories. During the advisory do not use water from the public water system for the dental unit, ultrasonic scaler, hand washing, or mixing disinfectants. Self-contained water units can be used with bottled water. Waterless hand hygiene products can be used for washing hands or bottled water and soap for visibly contaminated hands. As we have had boil water advisories in the recent past in Arizona, this is a great resource for us.
Aseptic technique for parenteral medications. The guidelines stress that intravenous (IV) tubings, bags, connections, needles, and syringes are single use only. Single dose vials are not to be used for multiple patients nor should leftover contents be combined for later use.
Oral surgical procedures. Since 1986 the dental guidelines recommended the use of sterile water or saline for a coolant/irrigant for surgical procedures involving the cutting of soft tissue or bone. This includes the incision, excision, or reflection of tissue that exposes normally sterile areas of the oral cavity. Examples include biopsy, periodontal surgery, implant surgery, apical surgery, and surgical extractions of teeth. The 2003 guidelines expand on this premise and also caution that dental units should be bypassed and single-use disposable or sterilizable tubing be used to deliver sterile surgical irrigation.
Sterilization and disinfection of patient-care items. This area is covered extensively in the guidelines. It remains an area of concern. In the past two years alone, it has been reported that thousands of dental patients from three different United States Veterans Administration hospitals have been exposure to bloodborne pathogens by inadequate sterilization and disinfection processing. It is vital that the licensed dental professionals in each practice supervise these procedures to ensure that the standard of care is being met.
Sterilization monitoring. In the 1986 guidelines, weekly biological monitoring (spore testing) of the sterilizers was recommended. In the 1993 guidelines, the placement of chemical indicators on the outside of each package was suggested. In the 2003 guidelines, placing chemical indicators both inside and outside of each package was recommended. However, it is rare that I see chemical indicator placement inside dental packaging when auditing dental facilities. In addition, since 2006, the Association for the Advancement of Medical Instrumentation (AAMI) has published standards that suggest that more sensitive class 5 chemical indicators (CI) that are now available may be used with each load as part of load release criteria for nonimplant loads. What this means is that if the class 5 CI shows a failure, the load should not be released for use. This works to narrow the gap between biological monitoring and obtaining the results, reducing the risk of releasing non-sterile instruments for patient care. It is a small investment to insure your risk management levels remain low.
Tuberculosis (TB). The 2003 dental guidelines thoroughly address TB. In addition, the 2005 CDC Guidelines for Preventing the Transmission of Mycobacterium tuberculosis in Health-Care Settings10 include dental practices in their scope. This means you should have a TB plan for your practice and, at the least, provide baseline skin testing of all employees. Fortunately, within the past year, a new rapid molecular test for TB drug-susceptibility has been made available that can determine within one to two days the appropriate medications to give for treating each individual patient. The older methods of testing could take as long as eight weeks.11 This new development is being used to treat TB more quickly and effectively and reduce the possibility of antibiotic resistance. New TB cases continue to decline each year in the United States.
The Future
 Will there be more regulation in the future? Probably. Presently infection control guidelines and requirements are widely acknowledged, but compliance, surveillance, and oversight are left to each individual employer. OSHA is concerned that there are significant gaps in compliance. On May 6, 2010, our Federal OSHA published Proposed Rules to deal with this issue. In this proposal, concern was noted that compliance was lacking in non-hospital healthcare settings. There also was the premise that perhaps there is not enough protection from airborne infectious diseases. A comment period was established and the deadline has passed, but there is yet to be a new law published. Sounds like there will be more required record keeping and proof that healthcare workers are being protected.
Will there be more regulation in the future? Probably. Presently infection control guidelines and requirements are widely acknowledged, but compliance, surveillance, and oversight are left to each individual employer. OSHA is concerned that there are significant gaps in compliance. On May 6, 2010, our Federal OSHA published Proposed Rules to deal with this issue. In this proposal, concern was noted that compliance was lacking in non-hospital healthcare settings. There also was the premise that perhaps there is not enough protection from airborne infectious diseases. A comment period was established and the deadline has passed, but there is yet to be a new law published. Sounds like there will be more required record keeping and proof that healthcare workers are being protected.It is interesting to note that a recent report from The Association of Occupational Health Professionals in Healthcare has named bloodborne pathogen exposure, safe patient handling, respiratory protection, and workplace violence as its top four safety concerns.13
In Conclusion
The guidelines and the tools are now available to have a successful infection prevention program that will in turn help reduce adverse outcomes. Want more information on the above topics? Go online to our AZDA.org website and go to the continuing education section. I have gone into detail in several separate articles expanding on most of the subjects listed above. If you want to, take the time to take the tests and get Infection Control/Infectious Disease continuing education hours for your license. Now we know what we have to do. Let’s do it. Keep your standards high and your risk management low. You know my mantra:References:
- Centers for Disease and Control and Prevention. Vital Signs: Central Line—Associated Blood Stream Infections ---United States, 2001, 2008, 2009. Morbidity and Mortality Weekly Report (MMWR) March 4, 2011/ 60(08);243-248, http://www.cdc.gov/mmwr/preview/mmwrhtml/mm6008a4.htm
- Centers for Disease and Control and Prevention. Reduction in Central Line-Associated Bloodstream Infections Among Patients in Intensive Care Units --- Pennsylvania, April 2001--March 2005 Morbidity and Mortality Weekly Report (MMWR)October 14, 2005 / 54(40);1013-1016 http://www.cdc.gov/mmwr/preview/mmwrhtml/mm5440a2.htm
- Centers for Disease and Control and Prevention. 2011 Guidelines for the Prevention of Intravascular Catheter-Related Infections. Healthcare Infection Control Practices Advisory Committee (HICPAC). April 1, 2011. http://www.cdc.gov/hicpac/pdf/guidelines/bsi-guidelines-2011.pdf
- Occupational Safety and Health Administration (OSHA). Bloodborne pathogens. - 1910.1030 http://osha.gov/pls/oshaweb/owadisp.show_document?p_table=STANDARDS&p_id=10051
- Centers for Disease Control and Prevention. Guidelines for Infection Control in Dental health-Care Settings---2003: Morbidity and Mortality Weekly Report (MMWR) December 19, 2003 / 52(RR17);1-61 http://www.cdc.gov/mmwr/preview/ mmwrhtml/rr5217a1.htm
- Centers for Disease Control and Prevention. Recommended Infection-Control Practices for Dentistry. MMWR Morb Mortal Wkly Rep 1986; 35: 237-242.
- Centers for Disease Control and Prevention. Recommended infection-Control Practices for Dentistry, 1993. MMWR Morb Mortal Wkly Rep 1993; 42: 1-12.
- Centers for Disease and Control and Prevention. Updated Recommendations for Use of Tetanus Toxoid, Reduced Diphtheria Toxoid, and Acellular Pertussis (Tdap) Vaccine from the Advisory Committee on Immunization Practices 2010. Morbidity and Mortality Weekly Report (MMWR) January 14, 2011 / 60(01);13-15 http://www.cdc.gov/mmwr/preview/mmwrhtml/mm6001a4.htm?s_cid=mm6001a4_w
- Centers for Disease and Control and Prevention. Guideline for Hand Hygiene in Health-Care Settings Recommendations of the Healthcare Infection Control Practices Advisory Committee and the HICPAC/SHEA/APIC/IDSA Hand Hygiene Task Force Morbidity and Mortality Weekly Report (MMWR) October 25, 2002 / Vol. 51 / No. RR-16 http://www.cdc.gov/mmwr/PDF/rr/rr5116.pdf
- Centers for Disease and Control and Prevention. Guidelines for Preventing the Transmission of Mycobacterium Tuberculosis in Health-Care Settings, 2005. Morbidity and Mortality Weekly Report (MMWR) December 30, 2005 / 54(RR17);1- 141. http://www.cdc.gov/mmwr/preview/mmwrhtml/rr5417a1.htm?s_cid=rr5417a1_e
- Centers for Disease and Control and Prevention. Report of Expert Consultations on Rapid Molecular Testing to Detect Drug-Resistant Tuberculosis in the United States. http://www.cdc.gov/tb/topic/laboratory/rapidmoleculartesting/introduction.htm
- Federal Register /Vol. 75, No. 87 /Thursday, May 6, 2010 / Proposed Rules. http://osha.gov/FedReg_osha_pdf/FED20100506.pdf
- http://ohsonline.com/articles/2011/02/28/aohp-sayssharps-injuries-underreported.aspx?admgarea=news

